Estimating excess deaths in Indiana

Not only is excess mortality in Indiana evident across age groups, it is also a significant problem among each of the most common causes of death.
One of the most troubling trends facing the United States is that our life expectancy has long been lower than that of other comparable nations, and that this gap continues to widen at an alarming rate. One analysis that compared the U.S. to a group of 16 other high-income countries, for instance, showed that the difference in life expectancy between the U.S. and this peer set grew from 1.9 years in 2010 to 3.1 years in 2018.1
The sobering truth for us Hoosiers is that Indiana is among a group of states most responsible for the nation’s poor performance in this measure.2 In 1992, Indiana’s life expectancy was identical to that of the U.S., but by 2008 the difference between these two had grown to one full year. Over the next decade—a period during which Indiana life expectancy peaked and then began to decline—this gap widened to two years. Both Indiana and the U.S. saw a dramatic slide in this measure in 2020 as COVID-19 took a heavy toll, but the disparity between these two held steady (see Figure 1).
Figure 1: Life expectancy at birth, 1960 to 2020
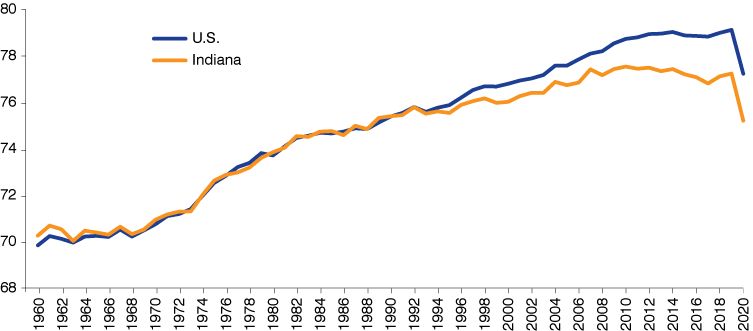
Sources: For 1960 to 2019, United States Mortality Database. University of California, Berkeley (USA). Available at usa.mortality.org. For 2020, Indiana Business Research Center, using data from the National Center for Health Statistics
One way to add context to lagging life expectancy figures is to estimate the number of excess deaths that places like the U.S. or Indiana have in a year due to their comparatively high mortality rates. Excess deaths simply measure the difference between the actual number of deaths in a given area and the number of deaths that this area would expect if it had different age- and gender-specific mortality rates (e.g., from some comparison region or from a different time period). For example, using the average mortality rates from a peer group consisting of the five most populous countries in Europe, a recent study showed that the U.S. had an estimated 417,500 excess deaths for its population under the age of 75 in 2017.3 This number accounted for nearly one-third of all deaths in that age group.
In this article, we will use a similar approach to estimate excess deaths in Indiana for the population under the age of 75. Rather than look to an international comparison, however, we will use average age-and gender-specific mortality rates from relatively high-performing areas of the U.S. as the peer region. Specifically, we will use average mortality rates from the four Census divisions—the Pacific, New England, Middle Atlantic and Mountain areas—that had life expectancies in 2019 that were above the U.S. mark of 79.1 (see Figure 2).
Figure 2: Life expectancy at birth by Census Division, 2019
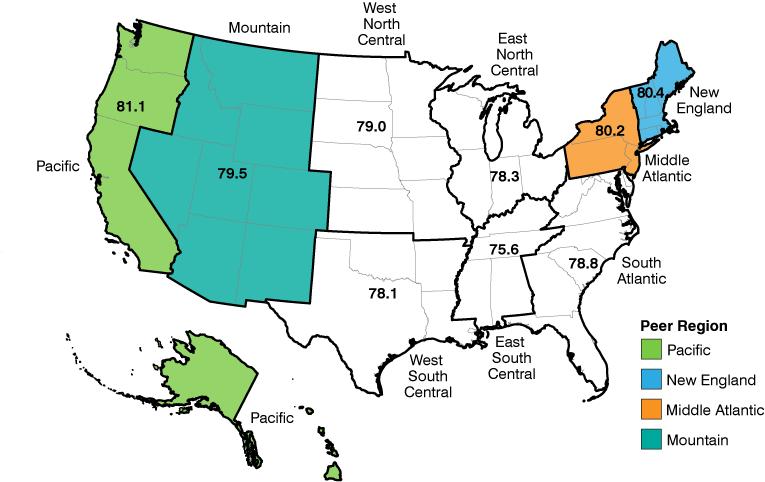
Source: United States Mortality Database. University of California, Berkeley (USA). Available at usa.mortality.org
Since the method used here to measure excess mortality is dependent on the geographic areas selected as the reference region, the estimates provided in this article should not be viewed as precise counts of preventable deaths in Indiana. A different peer region would yield different results.
A recent study from the CDC examining excess mortality from certain causes of death, for instance, used the three best-performing states for each cause as their reference regions, resulting in higher estimates of excess deaths in Indiana than we show here.4 By contrast, the peer region used in this analysis consists of 22 states that accounted for 41% of the U.S. population in 2020. Given this comparatively large peer region, the estimates presented here—while still striking—are also relatively conservative.
The bulk of this article will focus on mortality rates and excess deaths for the state’s population under the age of 75 between 2001 and 2019 to show that this is both a longstanding and wide-ranging problem in Indiana, as well as one that has grown progressively worse over the last two decades. Later—relying on a different approach to estimating excess mortality—we will briefly examine trends in Indiana during the COVID-19 pandemic.
Indiana mortality rates before the pandemic
Table 1 shows that Indiana’s mortality rates have long lagged the peer region, with the gaps between the two widening across all age groups. The most startling shift over this period has been the state’s 33% jump in mortality for the 25-to-44 age group—an increase driven largely by a sharp rise in substance abuse-related deaths. With the peer region experiencing just a 2% increase for this group over the same span, the gap in this measure between the two grew from 9% higher in Indiana in 2001 to 42% in 2019.
Table 1: Mortality rates by age group
| Mortality Rates, 2001 | Mortality Rates, 2019 | |||||
|---|---|---|---|---|---|---|
| Age Groups | Peer Region | Indiana | % Difference | Peer Region | Indiana | % Difference |
| < 1 year | 618 | 790 | 28% | 454 | 691 | 52% |
| 1 to 14 years | 19 | 25 | 29% | 14 | 19 | 40% |
| 15 to 24 years | 70 | 84 | 21% | 62 | 84 | 35% |
| 25 to 44 years | 141 | 153 | 9% | 144 | 204 | 42% |
| 45 to 64 years | 589 | 675 | 14% | 505 | 687 | 36% |
| 65 to 74 years | 2,245 | 2,678 | 19% | 1,575 | 2,093 | 33% |
Note: Mortality rates represent the number of deaths per 100,000 residents and are three-year averages (e.g., 2019 is an average of 2017 to 2019)
Source: National Center for Health Statistics, CDC Wonder database
Over this same period, Indiana also saw a slight uptick in mortality in the 45-to-64 age group while the rate for Hoosiers ages 15 to 24 was essentially unchanged. In these same groups, the peer region had declines of 14% and 11%, respectively.
Even in age groups where Indiana mortality rates have improved, the state continues to lose ground. This is most notable for the state’s infant population. Indiana’s infant mortality rate declined nearly 13% between 2001 and 2019, yet the peer region experienced a 26% improvement over the same period. So even though Indiana has seen modest progress in this measure, the state’s infant mortality rate was more than 50% higher than the peer region in 2019, up from a gap of 28% in 2001.
Excess mortality between 2001 and 2019
Table 2 shows how these wide differences in mortality rates translate into estimates of excess deaths in Indiana. In total, Indiana had an average of nearly 8,100 excess deaths per year between 2017 and 2019 for its population under the age of 75. This level of excess mortality means that 26% of all Indiana deaths in this age group could be considered potentially preventable. Excess mortality is most pronounced among Indiana’s youngest residents, where 34% of infant deaths were above the expected level. Moreover, excess mortality accounted for at least one-quarter of the state’s total deaths in each of these major age groups over this period.
Table 2: Indiana excess deaths by age group, 2017 to 2019 average
| Age Group | Actual Deaths | Expected Deaths | Excess Deaths | Excess Deaths as a Share of Indiana Total |
|---|---|---|---|---|
| <1 | 560 | 368 | 192 | 34% |
| 1 to 14 | 233 | 167 | 66 | 28% |
| 15 to 24 | 777 | 573 | 204 | 26% |
| 25 to 44 | 3,391 | 2,375 | 1,016 | 30% |
| 45 to 64 | 12,867 | 9,503 | 3,364 | 26% |
| 65 to 74 | 12,915 | 9,691 | 3,224 | 25% |
| Total (ages 0 to 74) | 30,743 | 22,677 | 8,066 | 26% |
Notes: Expected deaths are calculated by applying mortality rates from the peer region to the Indiana population in each age group. Excess deaths are the difference between actual deaths and expected deaths.
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
As Figure 3 highlights, excess mortality in Indiana has increased in each of these age groups since 2001. By far the most significant shift over this period has occurred among younger adults. In 2001, excess mortality accounted for only 8% of all Hoosier deaths in the 25-to-44 age group. However, this measure has climbed to 30% by 2019. The next-largest jumps were in the 45-to-64 age group and among infants.
Figure 3: Indiana excess deaths as a share of total deaths by age group
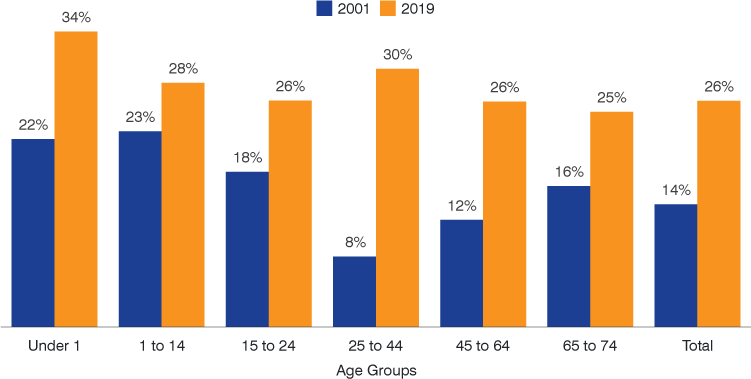
Note: Values are three-year averages (e.g., 2019 is an average of 2017 to 2019)
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
Taking the longer view, Indiana's excess mortality share for the population under age 75 was generally below 5% until the mid-1990s, but has since been on a steep and steady climb (see Figure 4).
Figure 4: Indiana excess deaths as a share of total deaths for population under age 75, 1970 to 2019
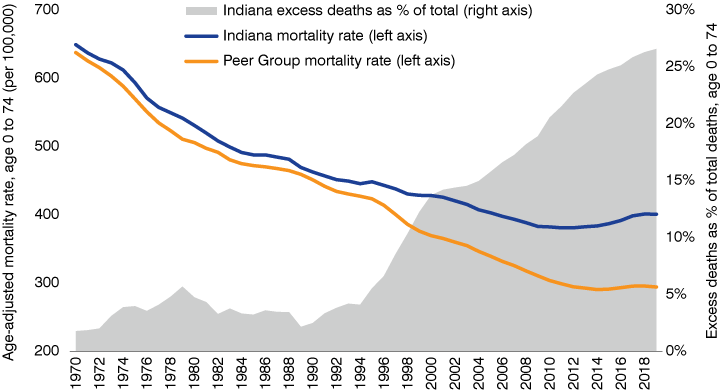
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
Note: Mortality rates and excess death shares are three-year averages (e.g., 2019 is an average of 2017 to 2019). Excess death shares are derived from age-adjusted mortality rates for the 0-to-74 age group
Excess mortality for leading causes of death
Not only is excess mortality in Indiana evident across age groups, it is also a significant problem among each of the most common causes of death. As Table 3 shows, excess mortality accounts for at least 20% of all deaths from each of the six leading causes for Indiana’s population under age 75. Most notably, roughly half of Hoosier deaths from chronic lower respiratory diseases (CLRD)—which are conditions linked largely to smoking—should be considered potentially preventable. In terms of absolute numbers, the 1,730 excess deaths per year from heart disease topped the list over this period.
Table 3: Indiana excess deaths by leading causes of death, 2017 to 2019 average
| Cause | Actual Deaths | Expected Deaths | Excess Deaths | Excess Deaths as a Share of Indiana Total |
|---|---|---|---|---|
| Cancer | 7,780 | 6,190 | 1,590 | 20% |
| Heart Disease | 5,846 | 4,116 | 1,730 | 30% |
| Chronic lower respiratory disease | 1,939 | 979 | 960 | 49% |
| Drug Overdose | 1,707 | 1,307 | 400 | 23% |
| Diabetes | 1,143 | 833 | 310 | 27% |
| Stroke | 1,013 | 733 | 280 | 27% |
Note: Excess deaths and expected deaths are derived from differences between Indiana and the peer region in age-adjusted mortality rates by cause for the 0-to-74 age group
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
For causes such as cancer, heart disease and stroke, the story for Indiana relative to the peer region is like the trends in infant mortality. That is, Indiana’s mortality rates from these causes are improving, just not improving as rapidly as in the peer region. As a result, excess mortality as a share of total deaths from these causes has increased over the last two decades, even though the state’s mortality rates have declined.
Indiana’s mortality rates from CLRD, however, did not improve at all between 2001 and 2019 while the peer region saw a 30% decline in this measure, leading to near doubling of Indiana’s excess mortality share from this cause over the last two decades (see Figure 5 ).
Figure 5: Indiana excess deaths as a share of total deaths by select causes
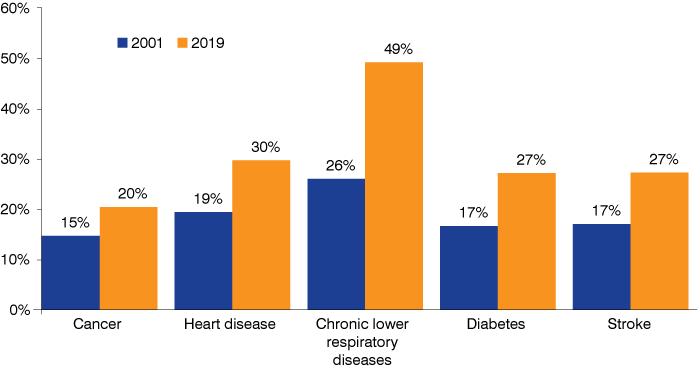
Note: Values are three-year averages (e.g., 2019 is an average of 2017 to 2019). Excess deaths and expected deaths are derived from differences between Indiana and the peer region in age-adjusted mortality rates by cause for the 0-to-74 age group
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
With respect to drug overdose deaths, this exercise of estimating excess mortality does not seem to do the problem justice. As is well known, drug addiction and overdoses in the U.S. is a national crisis. While Indiana is certainly among the hardest-hit states, few areas of the country have gone unscathed.
In the peer region, for example, overdose-related mortality rates roughly tripled between 1999 and 2019 (see Figure 6 ). Two decades ago, Indiana was among the nation’s top performers in this measure, but by 2019 the state’s mortality rate from overdoses was 24% higher than in the peer region. In 2020, unfortunately, this situation grew far worse, with drug overdose deaths increasing by 37% in Indiana, and the state’s mortality rate from this cause 35% higher than the peer region.
Figure 6: Mortality rates from drug overdoses, 1999 to 2020
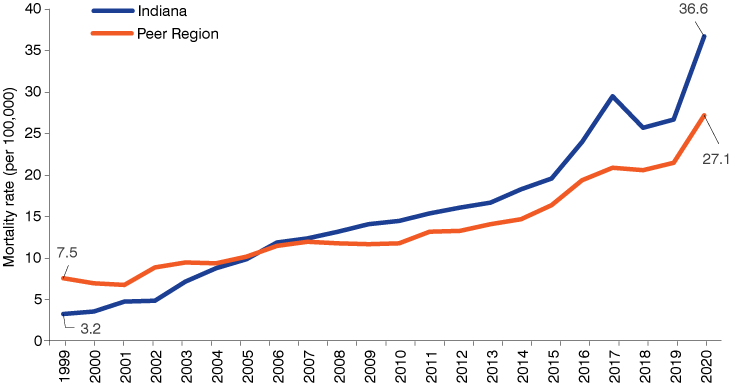
Note: Mortality rates represent the number of deaths per 100,000 and are age-adjusted
Source: National Center for Health Statistics, CDC Wonder database
Given that drug overdose mortality is an urgent crisis in both the peer region and Indiana, however, it does not seem appropriate to use one as the standard against which we assess the other. Instead, it’s better to view anything above the lowest levels of drug overdose deaths as excess mortality.
Geographic patterns of excess mortality
Indiana is not the only state in this part of the country to struggle with high mortality rates. In Kentucky, excess mortality accounted for nearly 37% of all deaths to residents under age 75 between 2017 and 2019. Ohio and Missouri also had excess mortality shares that were similar to Indiana’s over this period.
However, many Midwestern states have fared much better in this measure (see Figure 7) . Excess mortality in neighboring Michigan and Illinois is substantially lower than here in Indiana, while Iowa and Wisconsin have excess mortality shares below 10%. In Minnesota, “negative” excess mortality indicates that the state’s actual number of deaths were roughly 10% lower than would be expected based on the peer region’s rates. The wide disparity in excess mortality within the Midwest shows that geography is not destiny when it comes to this measure.
Figure 7: Excess deaths as a share of total deaths for the population under age 75 in select states, 2017 to 2019 average
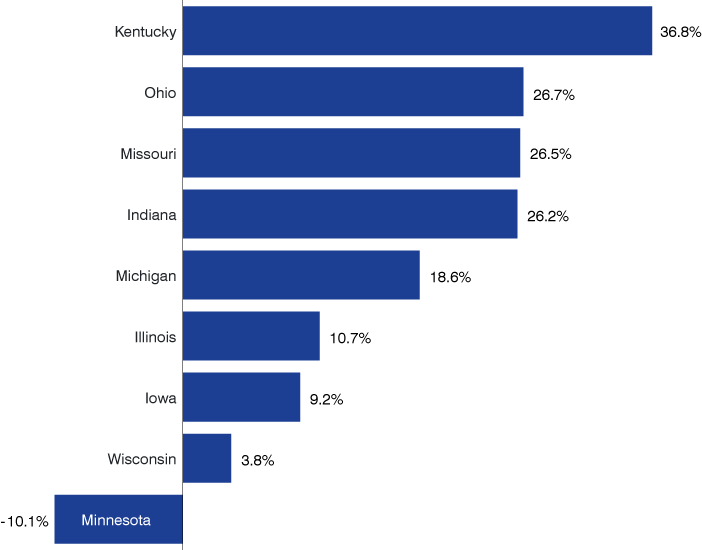
Note: Values derived from differences between each state and the peer region in age-adjusted mortality rates for the 0-to-74 age group
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
Looking around Indiana, ten counties had excess mortality shares above 40% over the 2017 to 2019 period, led by Scott County where more than half of all deaths to the population under age 75 are potentially preventable (see Figure 8 ). At the other end of the spectrum, only 4 of the state’s 92 counties outperformed the peer region. Hamilton County stands alone among this group with actual deaths over the 2017 to 2019 period 40% lower than the expected level, followed by Hendricks (-8.3%), Warren (-0.3%) and Monroe (-0.3%) counties.
Figure 8: Excess deaths as a share of total deaths for the population under age 75 by county, 2017 to 2019 average
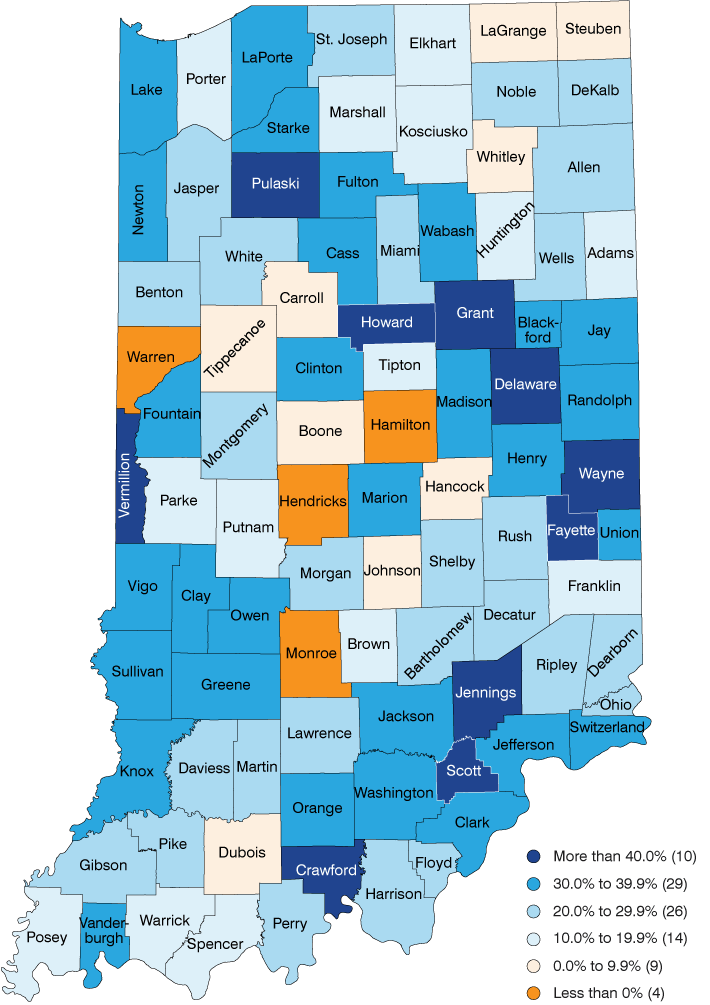
Note: Values derived from differences between each county and the peer region in age-adjusted mortality rates for the 0-to-74 age group
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
Excess mortality during the pandemic
In 2020, of course, everything changed with the onset of the COVID-19 pandemic. As Table 4 shows, COVID-19 was Indiana’s third-leading cause of death in 2020, with the number of deaths nearly twice as large as for CLRD, the state’s fourth-leading cause. Additionally, Indiana’s age-adjusted mortality rate for COVID-19 ranked 13th-highest among states in 2020.
Note that these data are based on the primary underlying cause of death listed on death certificates. It is likely, however, that COVID-19 was also a contributing factor in the uptick for some other causes of death in 2020 such as heart disease, diabetes and Alzheimer’s.5
Table 4: Indiana’s leading causes of death, all ages
| Deaths | Age-adjusted mortality rates | |||||
|---|---|---|---|---|---|---|
| Cause | 2018 to 2019 Average | 2020 | Change | 2018 to 2019 Average | 2020 | % Change |
| Heart Disease | 14,544 | 15,169 | 625 | 179.8 | 183.9 | 2% |
| Cancer | 13,497 | 13,664 | 167 | 164.6 | 162.7 | -1% |
| COVID-19 | 0 | 8,527 | N/A | 0 | 103.2 | N/A |
| Chronic lower respiratory disease | 4,631 | 4,529 | -102 | 56.6 | 53.7 | -5% |
| Stroke | 3,256 | 3,317 | 61 | 40.4 | 40.3 | 0% |
| Alzheimer's disease | 2,615 | 2,803 | 188 | 32.5 | 34.3 | 6% |
| Diabetes | 2,069 | 2,446 | 377 | 25.5 | 29.6 | 16% |
| Drug overdose | 1,661 | 2,318 | 657 | 26.1 | 36.6 | 40% |
| All other causes | 23,574 | 25,421 | 1,847 | 303.1 | 322.8 | 6% |
| Total | 65,847 | 78,194 | 12,347 | 828.6 | 967.1 | 17% |
Source: National Center for Health Statistics, CDC Wonder database
Given the sudden rise and rapid spread of COVID-19 throughout the country in 2020, the method of comparing Indiana to the peer region does not shed any light on the additional impacts that the pandemic had on excess mortality in the state. A better way to assess these additional impacts is to compare deaths in Indiana in 2020 to the state’s own average mortality for 2018 and 2019 (i.e., the years immediately preceding the pandemic). Also note that these estimates of excess mortality during the pandemic cover Indiana’s entire population, not just Hoosiers under the age of 75.
Due to these differences in approach, the estimates of excess mortality shown in Table 5 are not comparable to any of the earlier findings in this article. Instead, these estimates are largely just layered on top of Indiana’s already high levels of excess mortality.
In all, Indiana had roughly 11,000 excess deaths in 2020, with COVID-19 responsible for more than three-quarters of this total. The majority of the nearly 2,500 excess deaths from causes other than COVID-19 occurred in the 15-to-64 age group. In fact, Hoosiers between the ages of 25 and 44 had the largest share of excess mortality relative to total deaths in their age group, and nearly 90% of these excess deaths were from causes other than COVID-19.
Table 5: Indiana excess deaths by age group, 2020
| Excess Deaths by Cause | Age Group | Actual Deaths | Expected Deaths | COVID-19 | Other Causes | Total | Excess Deaths as a Share of Indiana Total |
|---|---|---|---|---|---|---|
| < 1 year | 527 | 540 | 0 | -13 | -13 | -2.5% |
| 1 to 14 | 245 | 224 | 0 | 21 | 21 | 8.6% |
| 15 to 24 | 916 | 765 | 10 | 141 | 151 | 16.5% |
| 25 to 44 | 4,226 | 3,373 | 108 | 745 | 853 | 20.2% |
| 45 to 64 | 14,722 | 12,729 | 1,041 | 952 | 1,993 | 13.5% |
| 65 to 74 | 15,725 | 13,864 | 1,653 | 208 | 1,861 | 11.8% |
| 75+ | 41,831 | 35,700 | 5,715 | 416 | 6,131 | 14.7% |
| Total | 78,192 | 67,195 | 8,527 | 2,470 | 10,997 | 14.1% |
Note: Expected deaths are calculated by applying Indiana’s average mortality rates from 2018 and 2019 to the state’s population in each age group in 2020. According to the CDC data, Indiana had 10 deaths from COVID-19 in its population under the age of 25, but the specific age groups for these cases are not reported. For the purposes of this table, we put these deaths in the 15-to-24 age group.
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
As Figure 9 shows, outside of COVID-19, drug overdoses were by far the leading cause of excess mortality in 2020 for Hoosiers between the ages of 15 and 64. These five leading causes accounted for 75% of all non-COVID-19 excess deaths in this age group.
Figure 9: Leading causes of excess mortality for Indiana’s population ages 15 to 64 (excluding COVID-19), 2020
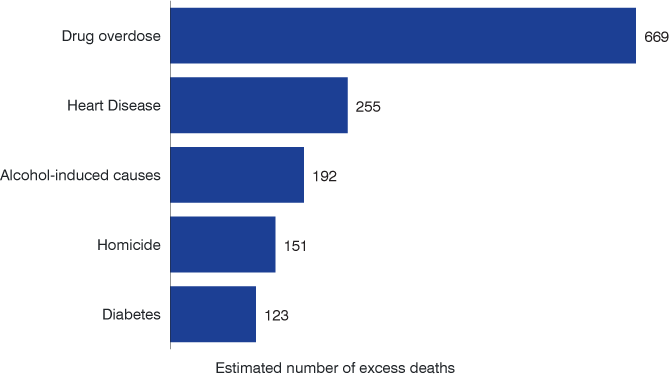
Source: Indiana Business Research Center, using data from the National Center for Health Statistics, CDC Wonder database
Conclusion
When Governor Eric Holcomb announced the creation of the Governor’s Public Health Commission in August 2021, he stated that public health was Indiana’s “Achilles’ Heel.”6 Surely there is no clearer evidence to support this statement than the scale and breadth of preventable deaths in the state. Young and old, urban and rural, across the spectrum of possible causes—we lose far too many Hoosiers every year, and this problem continues to trend in the wrong direction.
Public health crises have been at the top of mind in recent years—first with the ever-mounting epidemic of addiction and overdose, and more recently with COVID-19. These have both taken a heavy toll in Indiana, and rightly draw significant attention and resources. However, the state’s struggles with poor health are so pervasive and deeply rooted that even if we could largely alleviate these problems, Indiana would still lag most of the nation in most key health metrics.
Even in areas where Indiana has seen some improvement—such as the battles against infant mortality, cancer and heart disease—the state is still losing ground as gains elsewhere outpace our own. Any improvements are meaningful, of course, but we will know that the state of Hoosier health has truly begun to turn the corner when Indiana stops steadily falling behind better-performing areas of the country and begins to narrow these gaps.
Notes
- Steven H. Woolf, Ryan K. Masters, Laudan Y. Aron, “Effect of the covid-19 pandemic in 2020 on life expectancy across populations in the USA and other high income countries: simulations of provisional mortality data,” BMJ 2021; 373 :n1343 doi:10.1136/bmj.n1343
- Matt Kinghorn, “Indiana’s life expectancy falling further behind U.S.,” Indiana Business Review, Summer 2021, https://www.ibrc.indiana.edu/ibr/2021/summer/article1.html
- Samuel H. Preston and Yana C. Vierboom, “Excess mortality in the United States in the 21st century,” PNAS 2021 Vol. 118, no. 16 (April 12, 2021).
- Macarena C. Garcia, “Potentially excess deaths from the five leading causes of death in metropolitan and nonmetropolitan counties—United States, 2010 to 2017,” Morbidity and Mortality Weekly Report Vol. 68, no. 10 (November 8, 2019).
- “2020 Final Death Statistics: Covid-19 as an Underlying Cause of Death vs. Contributing Cause,” National Center for Health Statistics podcast transcript (January 7, 2022), www.cdc.gov/nchs/pressroom/podcasts/2022/20220107/20220107.htm
- Brandon Smith, “Governor Creates Public Health Commission to Recommend Health System Improvements,” Indiana Public Media, August 18, 2021, https://indianapublicmedia.org/news/governor-creates-public-health-commission-to-recommend-health-system-improvements.php
